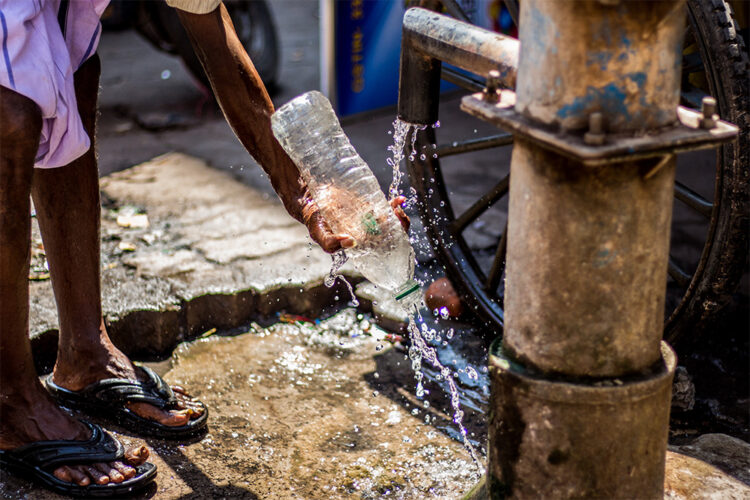New York: Escherichia coli (E. coli) and other disease-causing microbes are more likely to pass easily between humans and animals in countries, particularly low-income, where clean water, sanitation and hygienic controls are lacking, a new study suggests.
The continuous exchange, along with unregulated antibiotic use, leads to the emergence and spread of drug-resistant E. coli, said the researchers from the George Washington University in the US.
The team conducted the research in Cambodia’s Phnom Penh and identified multiple genetic elements that confer resistance to powerful antibiotics that were widely dispersed among humans and food production animals.
“The results from our study were jaw dropping. They suggested that E. coli strains from people and animals were exchanging DNA at rates that we don’t see in high-income countries. And the DNA that they were sharing makes them resistant to some of the most important antibiotics in human medicine,” said Lance B. Price, Professor of environmental and occupational health at the varsity.
“Countries that lack widespread access to clean water and other environmental controls could be inadvertently brewing the next pandemic,” Price added.
The study suggests that such environments create many opportunities for the exchange of bacteria and genetic elements that confer resistance to antibiotics. A lack of sewage treatment in rural settings can result in the contamination of drinking water for humans and animals.
“Ensuring consistent access to clean water and sanitation can improve people’s health and well-being in so many ways,” said Maya Nadimpalli, Assistant Professor of environmental health at Emory University Rollins School of Public Health.
“We’ve suspected that it could also help antibiotic resistance, but our findings show that improving access to clean water and sanitation is actually required — both in humans and food animals — if we want to have a fighting chance at preserving antibiotics for human health.”
The study showed that strains of E. coli in Phnom Penh had developed resistance to two powerful antibiotics used to treat humans — cephalosporins and fluoroquinolones.
People who are sickened by eating food or being exposed to drug-resistant E. coli and other microbes can develop life-threatening infections. Public health experts estimate that antibiotic resistant bacterial infections cause more than 1.3 million deaths worldwide each year.
In high-income countries like the US, experts focus on developing more effective antibiotics and getting people to avoid unnecessary antibiotic use.
However, this study suggests that the problem of antibiotic resistance will not go away unless public health officials address the lack of consistent access to basic sanitation and other environmental controls in countries where food animal production is intensifying.
(IANS)